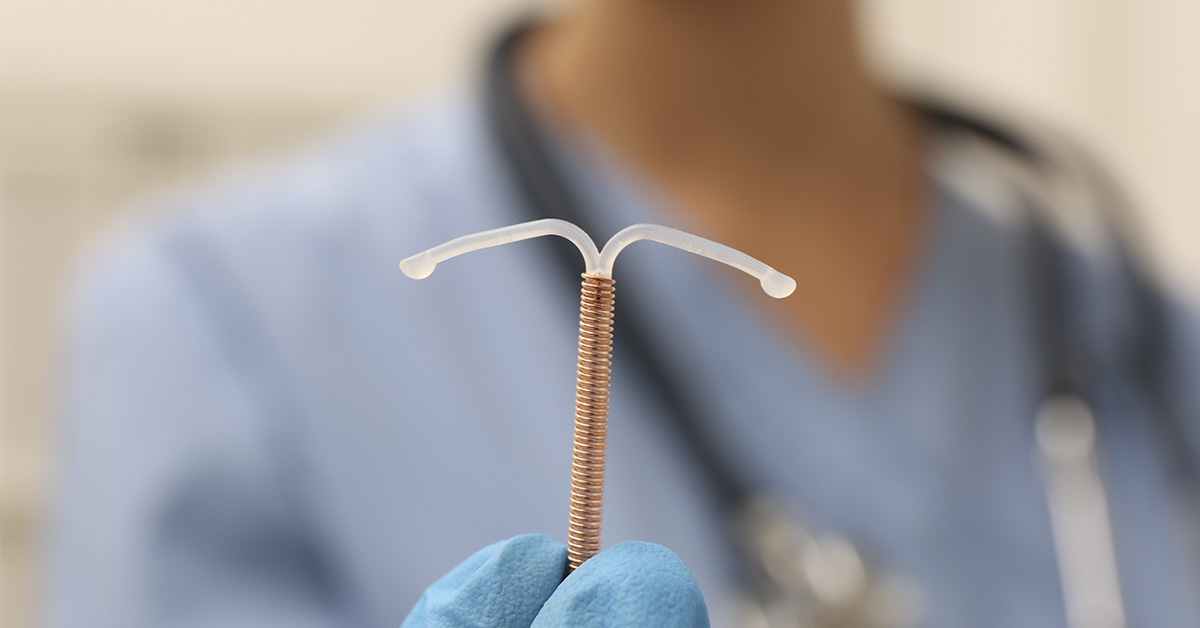
Queidy Araujo de Oliveira went in for a routine check on her IUD and left with news she never expected. Two years after having the copper device inserted, she was pregnant. Her son Matheus Gabriel was born in September 2025 at Hospital Sagrado Coracao de Jesus in Neropolis, Brazil. The pregnancy had been difficult, but Matheus arrived healthy. Moments after the baby was born, Dr Natalia Rodrigues picked up the failed IUD and placed it in his tiny hand. She then filmed him gripping it, then posted the video with a caption, “Holding my victory trophy: the IUD that couldn’t handle me!”
The clip spread quickly across social media, but the story attached to it wasn’t quite true. Matheus wasn’t born holding anything. Dr Rodrigues staged the shot after delivery, a detail she never hid, but one that got lost as the video was shared and reshared. Her actual point was a reminder that no contraceptive method is 100% effective.
Matheus is not the first baby to go viral because of being posed this way by a doctor.
The Photos That Keep Going Viral
In 2017, a photo of a newborn gripping a Mirena IUD circulated with the claim that he’d come out of the womb holding it. His mother, Lucy Tyler, posted the image herself with the hashtag #mirenafail and a note that the device had been found behind her placenta.
What she didn’t expect was how the story would mutate as it spread. A nurse had placed the IUD in her son’s hand after delivery, and her husband snapped the picture. By the time it went viral, that detail had disappeared. The baby was supposedly born clutching his mother’s failed birth control, a tiny victor against the odds.
That same year, a similar photo emerged from Vietnam. A 34-year-old mother of two who’d had her IUD for two years gave birth to a healthy boy, and medical staff posed him with the device for a picture. Dr Tran Viet Phuong, the attending physician, told local media outlet VnExpress International the shot was meant to be lighthearted. “I never thought it would receive so much attention,” she said. It did, and once again, the claim that the baby had been born holding the IUD spread faster than the correction.
The pattern repeats because the image is irresistible. A newborn baby defeating the very technology designed to prevent him, holding the evidence in his fist. It sounds like it could be true, which is exactly why it isn’t questioned. But the claim doesn’t just exaggerate what happened. It describes something that’s physically impossible.
Why Babies Can’t Be Born Holding an IUD
A baby doesn’t float freely inside the uterus during pregnancy. It grows inside the amniotic sac, a fluid-filled membrane that seals it off from the uterine wall, and the IUD sits outside this sac in the uterine cavity itself. The two spaces never connect.
Dr Sophia Yen, a Stanford clinical associate professor, explains that the fetus develops entirely within the amniotic sac, and the IUD can’t get inside it. There’s no moment during pregnancy when a baby could reach out and grab anything from the uterine cavity. Because the membrane keeps everything separate the entire time.
When the baby is delivered, the IUD might come out around the same time, pushed along by contractions or removed by medical staff afterwards, but it was never somewhere the baby could reach. These pregnancies happen not because the IUD fails to keep the baby out of its space but because it fails to prevent conception in the first place.
How IUDs Prevent Pregnancy
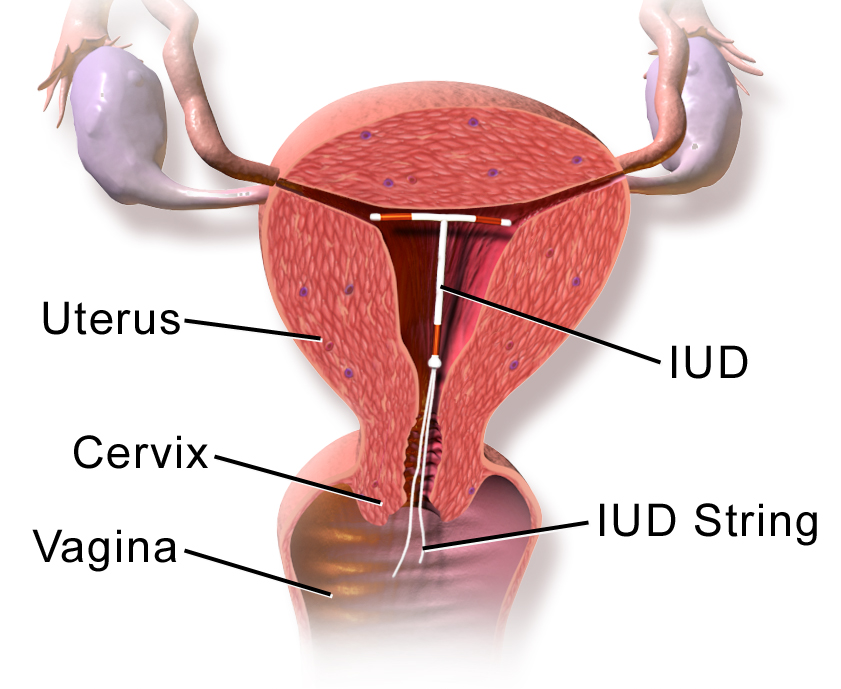
An IUD is a small T-shaped device that a healthcare provider inserts into the uterus, and once it’s in place, it prevents pregnancy for years without requiring anything from the user. No pills to remember, no supplies to buy, nothing to do until it’s time for removal.
There are two types. Copper IUDs contain no hormones and instead create an environment that’s toxic to sperm. The metal triggers an immune response that disables sperm before they can reach an egg, and it also changes the uterine lining to prevent implantation if fertilisation does occur. These last between five and ten years, depending on the brand.
Hormonal IUDs release progestin, a synthetic version of progesterone. This thickens the cervical mucus so sperm can’t get through and thins the uterine lining so a fertilised egg can’t attach. These last between three and seven years.
Both types rank among the most effective reversible contraceptives available. Fewer than 1% of users will become pregnant in the first year, according to the American College of Obstetricians and Gynaecologists. And hormonal IUDs like Mirena bring that number down to about 1 in 1,000, making them more effective than tubal ligation, birth control pills, patches, and rings. Compare that to the pill’s 9% failure rate with typical use and the advantage becomes clear. The IUD removes human error from the equation because once it’s in, there’s nothing to forget or misuse.
But no contraceptive is perfect, and when IUDs fail, it’s usually for the same few reasons.
Why IUDs Sometimes Fail
IUDs work best when they sit high in the uterine cavity, where they block sperm from reaching the fallopian tubes. But they can move, and when they do, they lose effectiveness.
Displacement is the most common cause of failure. Dr Steven Teo, a Singaporean obstetrician and gynaecologist, notes that this happens more often than people assume. “Most gynecologists would have seen a few cases during their career,” he said. Various factors can cause it, including sub-optimal insertion, heavy menstrual flow, or changes in the shape of the uterus over time.
Expulsion is when the IUD partially or completely falls out, which is most common in the first few months after insertion and can be related to uterine shape or a difficult insertion. Some people don’t notice when this happens, especially if it occurs during a heavy period. Perforation is rarer but more serious. This is when the device pushes through the uterine wall into the abdominal cavity, and in these cases, the IUD can’t prevent pregnancy because it’s no longer in the uterus at all.
Queidy Araujo de Oliveira had her copper IUD for two years before discovering she was pregnant, and while her doctors didn’t publicly confirm what went wrong, displacement or malposition are the likely explanations. The copper IUD she used has a failure rate of only 0.6%. But for someone in that small percentage, the statistics offer little comfort. The question becomes what to do next.
What Happens If You Get Pregnant With an IUD
Finding out you’re pregnant when you have an IUD means making decisions quickly. The device doesn’t belong in a pregnant uterus, and leaving it there carries risks that increase as the pregnancy progresses.
Doctors usually recommend removal when the strings are still accessible through the cervix, so they act before the risks increase. This creates a small chance of miscarriage because the area is disturbed, but doctors generally consider it riskier to remove the device. It can lead to infections, premature rupture of the amniotic sac, and bleeding, so doctors weigh those possibilities early. The chances of these complications are not enormous, but they exist, and they rise when the device stays in place. Once doctors remove the IUD, fertility returns right away and future pregnancies aren’t affected.
There’s also an increased risk of ectopic pregnancy when conception occurs with an IUD in place. This is when the fertilised egg implants outside the uterus. Usually in a fallopian tube, and it requires immediate medical attention.
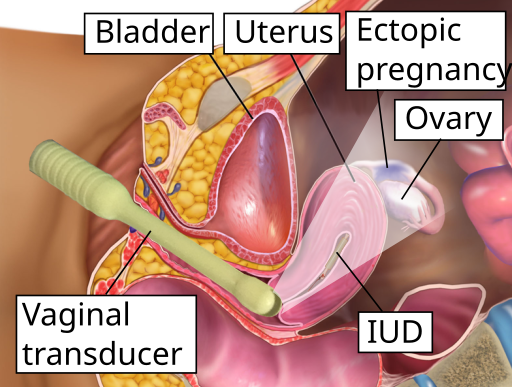
Anyone who suspects they might be pregnant while using one should see a doctor quickly to rule this out.
Sometimes removal isn’t possible. If the device has shifted to a position where pulling it would be dangerous, or if the strings are no longer reachable, the pregnancy may continue with it still inside. This is what happened to Queidy Araujo de Oliveira. Her doctors determined that removing the copper coil would put her unborn son at risk. So it stayed in place for all 9 months.
Queidy told local media outlet TV Anhanguera she experienced bleeding and detachments along the way, complications that can occur when a foreign object shares space with a developing fetus. Despite this, Matheus Gabriel arrived healthy.
Read More: 15 of the most raw, real, and amazing birth photos
How to Reduce Your Risk
Most IUD failures come down to position, which means catching a problem early can make the difference between effective contraception and an unplanned pregnancy.
Dr Steven Teo recommends getting a scan immediately after insertion to confirm the device is seated properly. Not all providers do this routinely, so you may need to ask. He also suggests annual check-ups to verify it’s still in a favourable position, though some providers only schedule follow-ups if you’re concerned. The UK’s National Health Service recommends a check at three to six weeks after insertion if your provider offers one, but this isn’t standard everywhere.
Between appointments, you can monitor things yourself by checking the strings monthly. These hang through the cervix and should be easy to feel. If you can’t find them, if they seem shorter or longer than usual, or if you can feel the hard plastic of the device itself, something may have shifted, and you should book an appointment.
Other warning signs include fever, unusual pain, abnormal discharge, or heavy bleeding. These could indicate infection or perforation, and you should seek an urgent appointment if they occur. Expulsion is most common in the first few months after insertion, so paying attention during this window matters most.
None of this guarantees prevention. The copper IUD Queidy used has a failure rate of just 0.6%, and she still got pregnant. But regular checks improve the odds, and knowing what to look for means you’re more likely to catch a problem before it becomes a pregnancy.
The Factory Is Closed
The video of Matheus Gabriel has now spread across thousands of social media accounts, and the same false claim follows it everywhere. The baby that was born gripping his mother’s failed IUD.
Doctors and nurses share these photos for a different reason. They want to show something genuinely remarkable, a pregnancy that fought to exist. Matheus held on for nine months while a copper device sat in the same uterus, working against him. His mother, Queidy Araujo de Oliveira, bled, faced complications, and still delivered a healthy son. He didn’t outsmart birth control. Nature found a way.
Dr Natalia Rodrigues shared the video to remind people that no contraceptive works every single time. Matheus exists because his mother landed in a 0.6% margin, and now he’s here. Healthy and presumably unaware that strangers once passed his photo around the internet.
His father had been waiting for a vasectomy when Queidy found out she was pregnant. After Matheus arrived, he posted online that “the factory is now closed.”
The family seems happy with how things turned out, even if the story strangers tell about them isn’t the one they actually lived.
Read More: Toddler with Birth Defect Melts Hearts After Showing his Dog he can Walk